- A biopsy is a sample of tissue taken from the abnormal area of tissue with a needle through the skin. This is done to find out if the tumour is cancer or not.
- A biopsy is generally only done if the results are going to change your treatment options or provide more information.
- If the biopsy shows the tumour is not cancer (benign) you may avoid surgery that you do not need.
- A biopsy can sometimes tell the type of cancer and how aggressive the cancer is. This may also change your treatment options.
- Some tumours are easier to biopsy than others due to their size and/or location in the kidney. Sometimes a biopsy is not able to tell if the tumour is cancer or not.
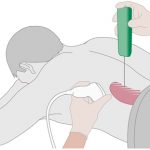
- A biopsy is most commonly done by a radiologist (doctor who reads x-rays, ultrasounds and CT scan) with freezing (numbing) with the patient awake, and is not a surgery.
- Some hospitals have more experience with biopsies of kidney tumours than others.
- Side effects are uncommon. Sometimes patients have bleeding or pain after a biopsy. Spreading of the tumour is not a concern with biopsy.
Ongoing monitoring as you go through treatment and in follow-up involves a certain number of tests, including laboratory tests and imaging techniques. It’s important to keep a copy of the test results available so they can be discussed with your healthcare team so that you clearly understand the meaning and their implications.
How is kidney cancer diagnosed?
Why do I still need annual scans after successful surgery?
- MRI
Magnetic resonance imaging (MRI) scan of the abdomen is similar to a CT scan. Under special circumstances, it may be better suited than a CT scan. It is devoid of radiation. MRI may be less accessible than CT scans.
- ULTRASOUND
An imaging procedure used to examine the internal organs of the abdomen, including the liver, gallbladder, spleen, pancreas, and kidneys. The blood vessels that lead to some of these organs can also be looked at with ultrasound. For example, an ultrasound of the heart (cardiac echo) can be performed prior to starting therapy to confirm good heart function. An ultrasound can be performed to look for liver metastases.
- BONE SCAN
A test performed with weak radioactive substances (at a hospital department of nuclear medicine) that can identify bone metastases.
- SKELETAL SURVEY
A series of x-rays of all bones that is used to look for bone metastases. Some bone metastases may not show on a bone scan.
- MUGA SCAN
A test performed with weak radioactive substances to examine heart function. It provides similar information to a cardiac echo (see Ultrasound).
- CHEST X-RAY
An x-ray of the chest, lungs, heart, large arteries, ribs, and diaphragm. A chest x-ray can be used to follow the extent of lung metastases. Alternatively, it may be used to ensure that the lungs are not damaged by some medications.
- PET SCAN
A positron emission tomography (PET) scan is an imaging test that uses a radioactive substance (called a tracer) to look for metastases. It identifies areas of the body that may harbour cells that are more active than usual. Cell activity may imply cancer activity. PET scans may therefore detect sites of metastases that cannot be otherwise detected by CT or MRI.
Kidney cancer can affect the levels of certain chemicals in the blood. Blood chemistry tests evaluate such things as electrolytes (sodium, potassium, chloride, bicarbonate), blood urea nitrogen (BUN), calcium, and creatinine. These substances indicate whether the patient can or cannot tolerate certain treatments. For example, some medications may affect renal function. Serum creatinine provides information on whether renal function is or is not adequate. These blood levels are routinely measured before and during therapy.
These tests assess levels of albumin, ALP (alkaline phosphatase), ALT (alanine transaminase), AST (aspartate aminotransferase), GGT (gamma-glutamyl transpeptidase), prothrombin time, serum bilirubin, and urine bilirubin. These substances indicate whether the patient’s liver can or cannot tolerate certain treatments. These are routinely measured before and during therapy.
- The number of red blood cells (RBCs)
- The number of white blood cells (WBCs)
- The total amount of hemoglobin in the blood
- The fraction of the blood composed of red blood cells (hematocrit)
- Average red blood cell size (MCV)
- Hemoglobin amount per red blood cell (MCH)
- The amount of hemoglobin relative to the size of the cell (hemoglobin concentration) per red blood cell (MCHC)
- Platelet count
These substances indicate whether the patient’s red blood cells (allow the functioning of all organs), white blood cells (immune cells) and platelets (coagulation) are adequate to tolerate certain treatments. These are routinely measured before and during therapy.
Analysis of substances present in the urine. Some medications may affect renal function and the presence of these substances may be detected in the urine. For example, protein is usually not present in the urine. Excessive amounts of protein may imply kidney damage.
Further details can be found at MedLine Plus (a service of the U.S. National Library of Medicine and the National Institutes of Health) at www.nlm.nih.gov by using the search term “renal cell carcinoma”.
WHAT DOES STAGE AND GRADE MEAN
Once a diagnosis of cancer has been made, the cancer is given a grade and a stage. This information helps you and your doctor choose the best treatment for you.
GRADE
Grade describes how the cancer cells look and behave compared to normal cells. Kidney cancer can be given a grade from 1 to 4. The lower the number, the lower the grade. Knowing the grade gives your healthcare team an idea of how quickly the cancer may be growing and how likely it is to spread. Lower grade cancer cells tend to be slow growing and are less likely to spread.
STAGE
Stage describes the tumour size and if it has spread. For kidney cancer, there are 4 stages. Each stage is given a number from 1 to 4. Generally, the higher the number, the more the cancer has spread. Early stage kidney cancer is stages 1, 2 and 3. Stage 4 kidney cancer is not early stage kidney cancer.
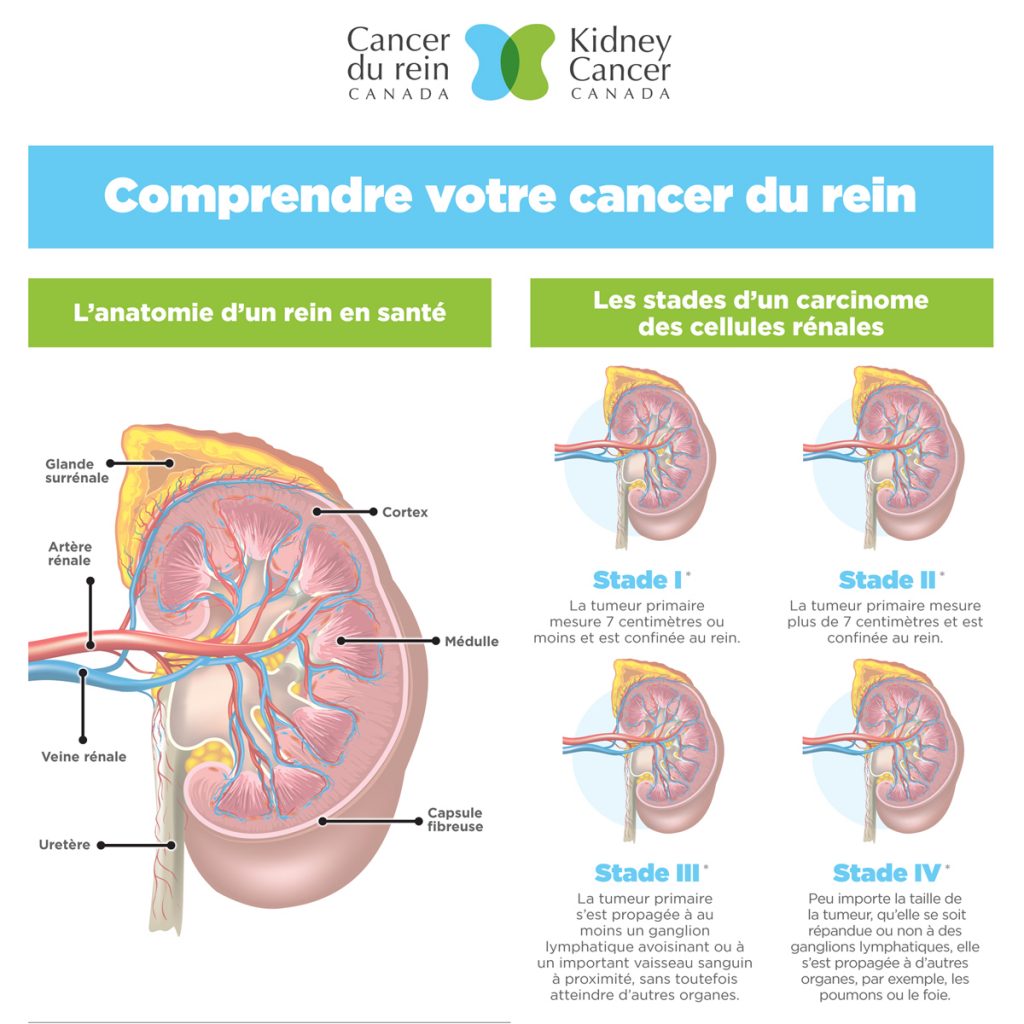
What each stage means:
- STAGE I
The tumour is fairly small, 7 cm or smaller, that has not spread beyond the kidney.
- STAGE II
The tumour is larger than 7 cm that has not spread beyond the kidney.
- STAGE III
The tumour has grown beyond the kidney (e.g., to the fatty tissue that surrounds the kidney) and/or cancer cells have entered 1 lymph node.
- STAGE IV
Cancer cells have spread to other organs (e.g. lungs, liver, bone) and/or cancer cells have spread to multiple (2 or more) lymph nodes. This stage is called metastatic kidney cancer and presence of kidney cancer in other organs or parts of the body are called metastases.
What is Stage I
kidney cancer?
What is Stage II
kidney cancer?
What is Stage III
kidney cancer?
What is Stage IV
kidney cancer?
WHAT DOES IT MEAN WHEN THE CANCER METASTASIZES?
The term ‘metastasize’ describes the spread of cancer beyond the original site of the cancer to other parts of the body. To understand how cancer metastasizes, it is helpful to review how cancer first occurs.
Cancer begins when normal kidney cells change, or mutate. These cancerous cells then begin to multiply at a much faster rate than normal cells would, and form a tumour.
Once a tumour is large enough, its cells begin to release a substance called vascular endothelial growth factor, or VEGF, which stimulates the surrounding blood vessels to grow. This process is referred to as angiogenesis. The increased blood supply enables the tumour to continue to grow, but also starts to carry tumour cells from the kidney throughout the rest of the circulatory system to other parts of the body, where new tumours may develop.
It is important to note that if a new tumour develops in a different area of the body – for example, in the lung – this is referred to as kidney cancer that has metastasized, not a new diagnosis of lung cancer.
Understanding the nature of kidney cancer, including how it metastasizes, helps to direct research into more effective treatments.
HOW STAGING AFFECTS TREATMENT
The exact sequence of steps in your treatment plan will be decided by your unique situation.
Usually, Stages I to III are initially treated by active surveillance, ablation therapy, surgery and/or Stereotactic Body Radiation Therapy (SBRT). However, in some cases a clinical trial may be offered for neo-adjuvant treatment (a treatment given as a first step to shrink a tumour before the main treatment) either before surgery, or immediately afterward (pembrolizumab).
Treatment for Stage IV kidney cancer, also called advanced or metastatic kidney cancer, may include active surveillance, surgery, systemic therapy, SBRT or a combination of one or more types of medical therapy.
SURGERY
Surgery is conducted to remove the kidney cancer situated within the kidney (requires removal of all or part of the affected kidney) and to remove all metastases (lymph nodes and other organs that have been affected, such as adrenal glands, intestine or part of lung or liver) that can be safely removed.
METASTATIC OR ADVANCED KIDNEY CANCER (STAGE IV)
- First-line therapy is the first medication used to treat a cancer. This is also called primary therapy or primary treatment.
- Second-line therapy is given when the first-line therapy doesn’t work, stops working, or has to be stopped because side effects are not being tolerated.
- Third-line therapy is given when both first- and second-line therapies don’t work, stop working, or have to be stopped due to side effects.
- Sequential therapy are not taken at the same time, but rather are taken one after the other. In Canada, treatment guidelines for kidney cancer make specific recommendations for first-, second- and third-line therapies for physicians to follow in treating patients with advanced kidney cancer.
SECTION REFERENCES:
- Biopsy
- What is the best treatment for my small kidney tumour? Ottawa Personal Decision Guide. October 14, 2019.
- Navigating tests and reports
- MedLine Plus: http://www.nlm.nih.gov/medlineplus/ency/article/000516.htm
- Definitions: MedLine Plus A.D.A.M. Medical Encyclopedia: http://www.nlm.nih.gov/medlineplus/encyclopedia.html